Type:
Educational Exhibit
Keywords:
Ischaemia / Infarction, Aneurysms, Diagnostic procedure, MR-Angiography, CT-Angiography, Catheter arteriography, Neuroradiology brain, CNS, Anatomy
Authors:
J. J. H. Lam, L. E. McAdory, C. L. Ho; Singapore/SG
DOI:
10.26044/ecr2019/C-0339
Findings and procedure details
Etiology and demographics
- There are four persistent fetal anastomoses between the carotid and vertebrobasilar circulations.
These represent the non-obliterated remnants of the pre-segmental dorsal arteries which comprise the persistent primitive trigeminal artery (PPTA),
persistent hypoglossal artery (PHA),
persistent otic (acoustic) artery (POA) and the proatlantal intersegmental artery (PIA). These primitive carotid vertebrobasilar anastomoses occasionally persist into adulthood and may be incidentally detected on imaging [1].
- In the early embryonic stage,
blood supply to the hindbrain is mainly via the 4 carotid-vertebrobasilar anastomoses.
These then regress within a week as the posterior communicating and vertebrobasilar arteries begin to develop (see Figure 1).
Rarely,
failure of regression of these primitive anastomoses occurs.
- Of the persistent fetal anastomoses,
the PPTA is the most common with a prevalence of 0.1-0.6% and represents up to 85% of the persistent embryological anastomoses [1-4].
- The PHA is the second most common carotid-vertebrobasilar anastomosis with a prevalence of 0.02-0.10% [5].
Clinical and imaging findings:
PPTA:
-
The PPTA originates from the internal carotid artery (ICA) distal to its exit from the carotid canal and forms an anastomosis with the basilar artery.
The basilar artery caudal to the anastomosis is usually diminutive [2].
As such,
the main blood supply to the posterior circulation is predominantly by the ICA via the PPTA.
Thus,
thromboembolic phenomena,
dissection or atherosclerotic disease of the ICA may result in posterior circulatory ischaemia.
-
The PPTA may be classified into the medial or lateral subtype,
both of which are equally common.
In the lateral subtype,
the PPTA follows a posterolateral course and is associated with the trigeminal nerve roots and neural structures.
In the medial subtype,
the PPTA courses posteromedially with an intra-sellar or trans-hypophyseal course.
As such,
the PPTA is in close proximity to the pituitary gland and mass effect on the pituitary stalk may result in hypopituitarism [6,
7].
Rarely,
patients may present with neurovascular conflict or cranial nerve compression syndromes involving the oculomotor,
trochlear or abducens nerves as the PPTA may closely be related to these nerves in its course. On the sagittal projections,
the configuration of the horizontal and vertical portions of the ICA as well as the proximal PPTA resembles the Greek symbol Tau as well as a trident,
thus giving rise to the Tau sign and trident sign respectively.
-
In Saltzman type 2,
the PPTA joins the basilar artery caudal to the origins of the superior cerebellar arteries and posterior circulatory blood supply is predominantly via the posterior communicating arteries rather than the PPTA [2,
3].
PHA
- The PHA usually originates from the cervical ICA distal to the carotid bifurcation between the C1 and C3 levels [8,
9].
- It courses through the enlarged hypoglossal canal before it anastomoses with the basilar artery [8,
9].
- Patients with PHA are typically asymptomatic although there are case reports of associated hypoglossal nerve paralysis and glossopharyngeal neuralgia [8,
9].
- The PHA is also a major supplier of the posterior circulation and disease/occlusion of the PHA may result in ischaemia of the posterior circulation and brainstem [8,
9].
Case 1:
A 71 year-old woman of Chinese origin presented initially with symptoms of bilateral upper visual field defects.
Clinical examination was otherwise unremarkable.
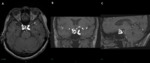
This was initially attributed to amaurosis fulgax or a transient ischaemic attack and a MRI of the brain was subsequently performed for further evaluation.
The MRI Brain demonstrated no evidence of an acute infarct.
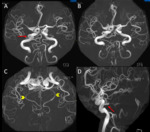
On the Time-of-flight magnetic resonance angiography,
a wide-necked saccular aneurysm was incidentally noted to arise from the cavernous right ICA,
with resultant expansion of the cavernous sinus and mass effect on the pituitary gland (Figures 3 and 4).
A persistent primitive trigeminal artery was also incidentally noted to arise just proximal to the right cavernous ICA aneurysm.
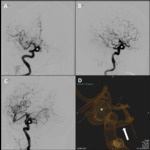
This was then further evaluated with a contrast enhanced CT Angiogram of the Circle of Willis (Figure 5) and conventional angiogram (Figure 6).
The basilar artery proximal to the carotid-vertebrobasilar anastomosis was hypoplastic and the bilateral superior cerebellar arteries were supplied by the PPTA.
Endovascular stenting of the aneurysm was considered but as the PPTA was in close proximity to the aneurysm,
there were potential risks for inadvertent occlusion of the PPTA at its origin with potential ischaemia of the posterior circulation.
This case highlights the importance of knowledge of the vascular anatomy of the PPTA as commonly,
the PPTA is associated with basilar artery hypoplasia and the majority of blood supply to the posterior circulation is from the ICA via the PTA.
As such,
occlusion of the ICA or PTA can result in posterior circulatory ischaemia.
The patient was thus conservatively managed.
Case 2:
A 74 year-old man with a history of diabetes mellitus and hypertension presented with progressive worsening dysphagia,
hoarseness of voice and intermittent fever of 2 months duration.
Clinical examination revealed erythema on the right side of the neck and a pulsatile mass with a bruit on auscultation.
Initial laboratory examination results revealed an elevated total white cell count and CRP levels with positive blood cultures of Salmonella.
In view of the clinical examination findings of a pulsatile mass,
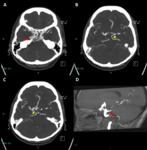
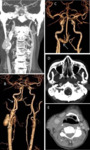
a CT neck and subsequent CT carotid angiogram was performed (see Figure 7) which revealed a large saccular aneurysm arising from the proximal right extra-cranial ICA just distal to the carotid bifurcation.
A persistent primitive hypoglossal artery was noted to arise distal to the origin of the aneurysm.
The bilateral vertebral arteries were hypoplastic and the PHA was the main supply to the posterior circulation.
Surgical resection of the aneurysm and graft replacement was subsequently performed.
Post-operatively,
the patient presented with left-sided hemiplegia.
A follow-up CT carotid angiogram revealed severe narrowing of the right carotid stent graft with reduced flow along the right ICA as well as the PHA (see Figure 8).
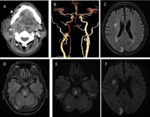
A MRI Brain was then performed which demonstrated multiple foci of acute infarcts in the territory of the right MCA as well as in the posterior circulation,
likely due to reduced flow from the PHA.
(see Figure 8).
He ultimately demised from sepsis.